Explore surgical options for infertility and understand when surgery may be the right solution for you (Consult your doctor for details)
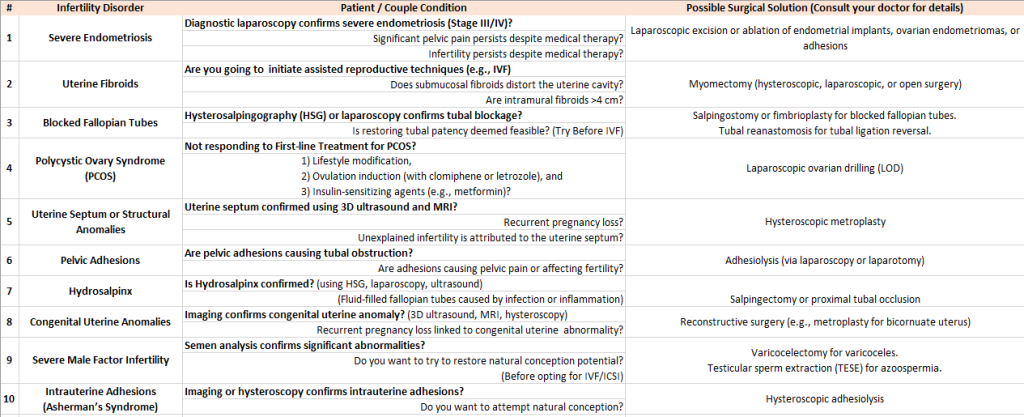
Infertility conditions which need Surgical Corrections
1) Endometriosis (Stages III & IV) 
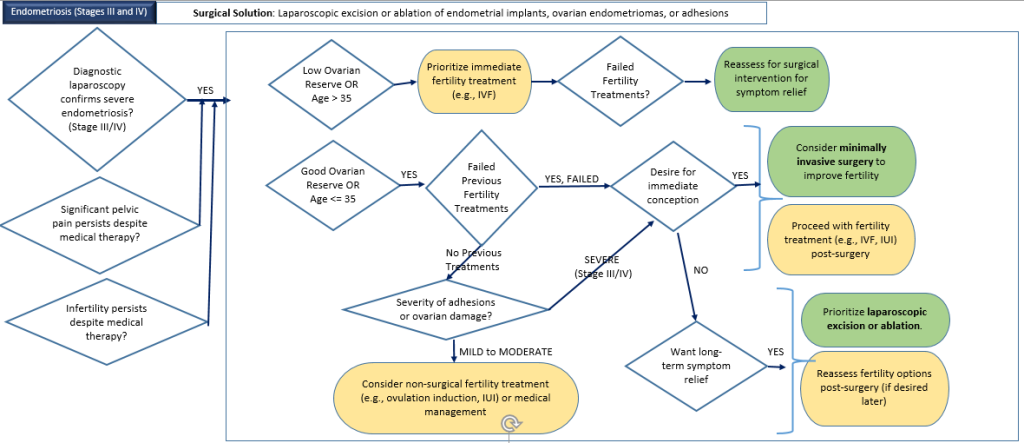
Description: A condition where tissue similar to the uterine lining grows outside the uterus, causing scarring and adhesions.
Symptoms: Severe pelvic pain, painful periods, pain during intercourse, infertility.
Diagnostic Methods: Diagnostic laparoscopy, transvaginal ultrasound, MRI.
Surgical Options Available: Laparoscopic excision or ablation of endometrial implants, adhesions, and ovarian endometriomas.
Alternative Treatments: Hormonal therapies (e.g., GnRH agonists), pain management, lifestyle changes.
Symptoms: Severe pelvic pain, painful periods, pain during intercourse, infertility.
Diagnostic Methods: Diagnostic laparoscopy, transvaginal ultrasound, MRI.
Surgical Options Available: Laparoscopic excision or ablation of endometrial implants, adhesions, and ovarian endometriomas.
Alternative Treatments: Hormonal therapies (e.g., GnRH agonists), pain management, lifestyle changes.
Potential Adversities of Delaying Surgery
Delaying surgery for endometriosis (Stages III and IV) can lead to:
1) Progressive scarring and adhesions, reducing the chances of natural conception and making future surgical correction more difficult.
2) Chronic pelvic pain, which may become resistant to medical treatment and negatively impact quality of life.
3) Reduced ovarian reserve, especially in women with existing low ovarian reserve or advanced maternal age, lowering the chances of successful fertility treatments.
4) Increased risk of organ involvement, such as bowel or bladder adhesions, leading to more complex surgical procedures and potential long-term complications.
5) Emotional and financial burden, due to repeated failed fertility treatments without addressing the underlying cause.
Delaying surgery for endometriosis (Stages III and IV) can lead to:
1) Progressive scarring and adhesions, reducing the chances of natural conception and making future surgical correction more difficult.
2) Chronic pelvic pain, which may become resistant to medical treatment and negatively impact quality of life.
3) Reduced ovarian reserve, especially in women with existing low ovarian reserve or advanced maternal age, lowering the chances of successful fertility treatments.
4) Increased risk of organ involvement, such as bowel or bladder adhesions, leading to more complex surgical procedures and potential long-term complications.
5) Emotional and financial burden, due to repeated failed fertility treatments without addressing the underlying cause.
2. Uterine Fibroids (Myomas) 
Description: Benign tumors in the uterus that can affect fertility and cause heavy bleeding.
Symptoms: Heavy menstrual bleeding, pelvic pain, infertility, recurrent miscarriages.
Diagnostic Methods: Transvaginal ultrasound, hysteroscopy, MRI.
Surgical Options Available: Myomectomy (hysteroscopic, laparoscopic, or open surgery).
Alternative Treatments: Uterine artery embolization, hormonal treatments.
Symptoms: Heavy menstrual bleeding, pelvic pain, infertility, recurrent miscarriages.
Diagnostic Methods: Transvaginal ultrasound, hysteroscopy, MRI.
Surgical Options Available: Myomectomy (hysteroscopic, laparoscopic, or open surgery).
Alternative Treatments: Uterine artery embolization, hormonal treatments.
Potential Adversities of Delaying Surgery
Increased Fibroid Size (Progressive Growth): Increased complexity of surgery, risk of hysterectomy
Heavy Menstrual Bleeding (Menorrhagia) & Anemia: Fatigue, blood transfusions, reduced quality of life
Infertility & Pregnancy Complications: Miscarriages, preterm birth, fetal growth restriction
Chronic Pelvic Pain & Pressure: Urinary issues, constipation, sciatic pain
Increased Risk of Degeneration & Acute Pain: Severe pain, necrosis, risk of infection
Risk of Malignancy (Leiomyosarcoma): Rare but possible transformation into cancer
Complications with Non-Surgical Treatments: Non-surgical treatments become ineffective
Increased Fibroid Size (Progressive Growth): Increased complexity of surgery, risk of hysterectomy
Heavy Menstrual Bleeding (Menorrhagia) & Anemia: Fatigue, blood transfusions, reduced quality of life
Infertility & Pregnancy Complications: Miscarriages, preterm birth, fetal growth restriction
Chronic Pelvic Pain & Pressure: Urinary issues, constipation, sciatic pain
Increased Risk of Degeneration & Acute Pain: Severe pain, necrosis, risk of infection
Risk of Malignancy (Leiomyosarcoma): Rare but possible transformation into cancer
Complications with Non-Surgical Treatments: Non-surgical treatments become ineffective
3. Blocked Fallopian Tubes 
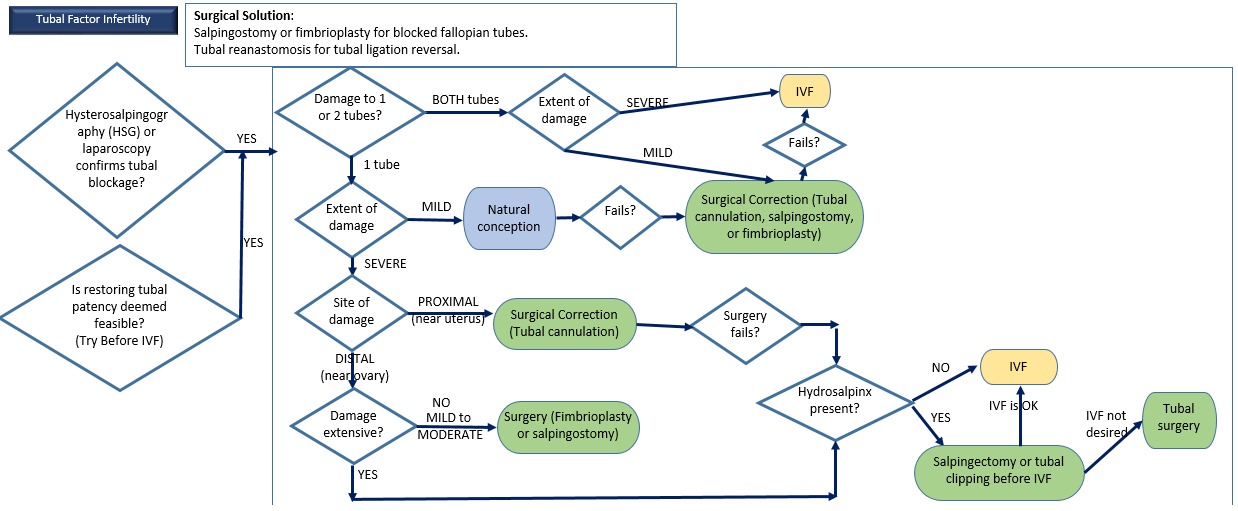
Description: Blockage in one or both fallopian tubes preventing fertilization.
Symptoms: Infertility, pelvic pain, irregular menstrual cycles.
Diagnostic Methods: Hysterosalpingography (HSG), laparoscopy.
Surgical Options Available: Salpingostomy, tubal reanastomosis, or tubal cannulation.
Alternative Treatments: IVF.
Symptoms: Infertility, pelvic pain, irregular menstrual cycles.
Diagnostic Methods: Hysterosalpingography (HSG), laparoscopy.
Surgical Options Available: Salpingostomy, tubal reanastomosis, or tubal cannulation.
Alternative Treatments: IVF.
Potential Adversities of Delaying Surgery
Delaying surgery for tubal factor infertility can lead to:
Progressive tubal damage, reducing the chances of successful repair.
Formation of hydrosalpinx, which negatively impacts natural conception and IVF outcomes.
Increased risk of ectopic pregnancy, especially if a partially blocked tube remains untreated.
Permanent infertility, particularly if both tubes are severely damaged or require removal.
Emotional and financial burden, due to repeated failed fertility treatments without addressing the underlying cause.
Delaying surgery for tubal factor infertility can lead to:
Progressive tubal damage, reducing the chances of successful repair.
Formation of hydrosalpinx, which negatively impacts natural conception and IVF outcomes.
Increased risk of ectopic pregnancy, especially if a partially blocked tube remains untreated.
Permanent infertility, particularly if both tubes are severely damaged or require removal.
Emotional and financial burden, due to repeated failed fertility treatments without addressing the underlying cause.
4. Polycystic Ovary Syndrome (PCOS) with Ovarian Drilling

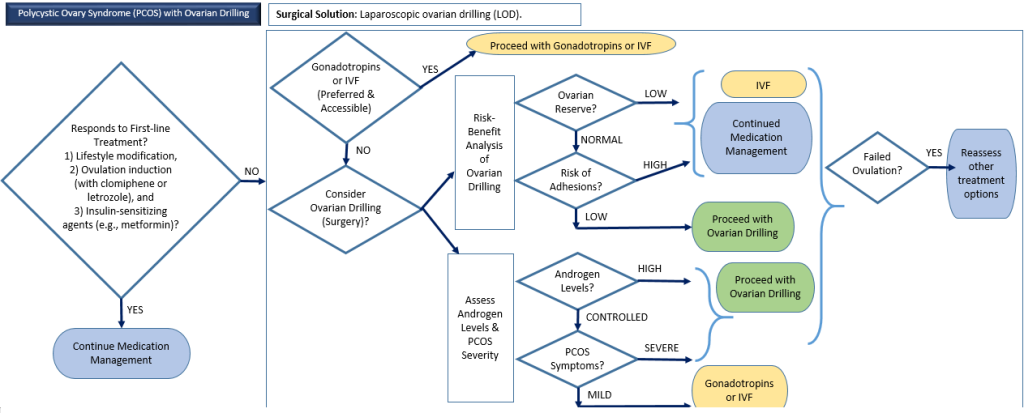
Description: A hormonal disorder causing enlarged ovaries with cysts.
Symptoms: Irregular periods, infertility, weight gain, acne, hirsutism.
Diagnostic Methods: Ultrasound, hormonal tests.
Surgical Options Available: Laparoscopic ovarian drilling.
Alternative Treatments: Lifestyle changes, ovulation induction (clomiphene or letrozole), metformin.
Symptoms: Irregular periods, infertility, weight gain, acne, hirsutism.
Diagnostic Methods: Ultrasound, hormonal tests.
Surgical Options Available: Laparoscopic ovarian drilling.
Alternative Treatments: Lifestyle changes, ovulation induction (clomiphene or letrozole), metformin.
Potential Adversities of Delaying Surgery
Delaying ovarian drilling or further treatment for PCOS can lead to:
Prolonged anovulation, resulting in delayed conception and increased risk of endometrial hyperplasia or cancer.
Worsening hormonal imbalance, leading to persistent symptoms of hyperandrogenism (hirsutism, acne, alopecia).
Increased metabolic risks, such as insulin resistance, Type 2 diabetes, obesity, and cardiovascular diseases.
Reduced fertility potential, particularly in women with low ovarian reserve or advanced maternal age.
Emotional and psychological distress, as repeated failed treatments without addressing the underlying issue may lead to anxiety, depression, and relationship stress.
Delaying ovarian drilling or further treatment for PCOS can lead to:
Prolonged anovulation, resulting in delayed conception and increased risk of endometrial hyperplasia or cancer.
Worsening hormonal imbalance, leading to persistent symptoms of hyperandrogenism (hirsutism, acne, alopecia).
Increased metabolic risks, such as insulin resistance, Type 2 diabetes, obesity, and cardiovascular diseases.
Reduced fertility potential, particularly in women with low ovarian reserve or advanced maternal age.
Emotional and psychological distress, as repeated failed treatments without addressing the underlying issue may lead to anxiety, depression, and relationship stress.
5. Uterine Septum or Structural Anomalies

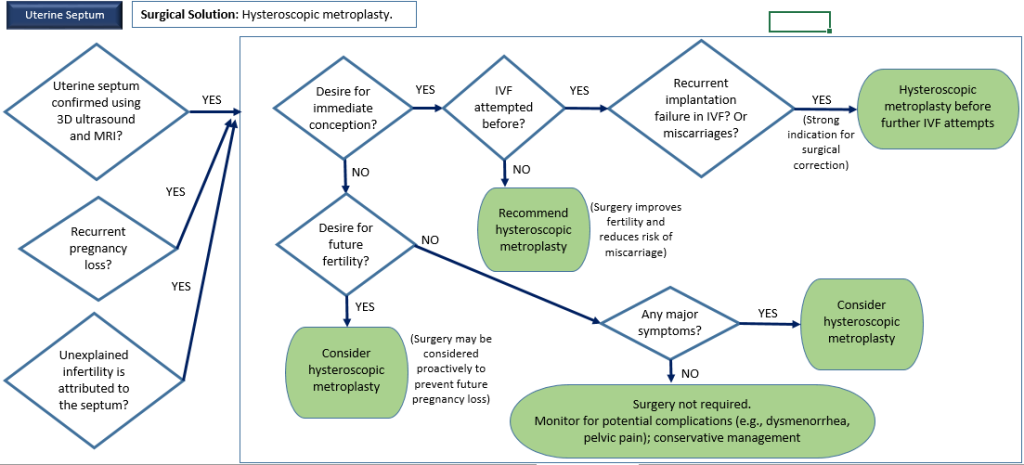
Description: Congenital malformations of the uterus affecting pregnancy.
Symptoms: Recurrent miscarriage, infertility, painful periods.
Diagnostic Methods: 3D ultrasound, MRI, hysteroscopy.
Surgical Options Available: Hysteroscopic metroplasty.
Alternative Treatments: IVF with embryonic monitoring (for specific cases).
Symptoms: Recurrent miscarriage, infertility, painful periods.
Diagnostic Methods: 3D ultrasound, MRI, hysteroscopy.
Surgical Options Available: Hysteroscopic metroplasty.
Alternative Treatments: IVF with embryonic monitoring (for specific cases).
Potential Adversities of Delaying Surgery
Delaying surgery for a uterine septum can lead to:
Recurrent pregnancy loss and increased risk of miscarriage or preterm labor.
Prolonged infertility, especially if the uterine septum is the primary cause.
Repeated IVF failures, resulting in emotional and financial strain.
Increased risk of uterine scarring (Asherman’s syndrome) from repeated miscarriages, which can further complicate fertility and pregnancy.
Missed opportunities for timely correction, leading to more complex pregnancies or reduced fertility in the future.
Delaying surgery for a uterine septum can lead to:
Recurrent pregnancy loss and increased risk of miscarriage or preterm labor.
Prolonged infertility, especially if the uterine septum is the primary cause.
Repeated IVF failures, resulting in emotional and financial strain.
Increased risk of uterine scarring (Asherman’s syndrome) from repeated miscarriages, which can further complicate fertility and pregnancy.
Missed opportunities for timely correction, leading to more complex pregnancies or reduced fertility in the future.
6. Pelvic Adhesions 
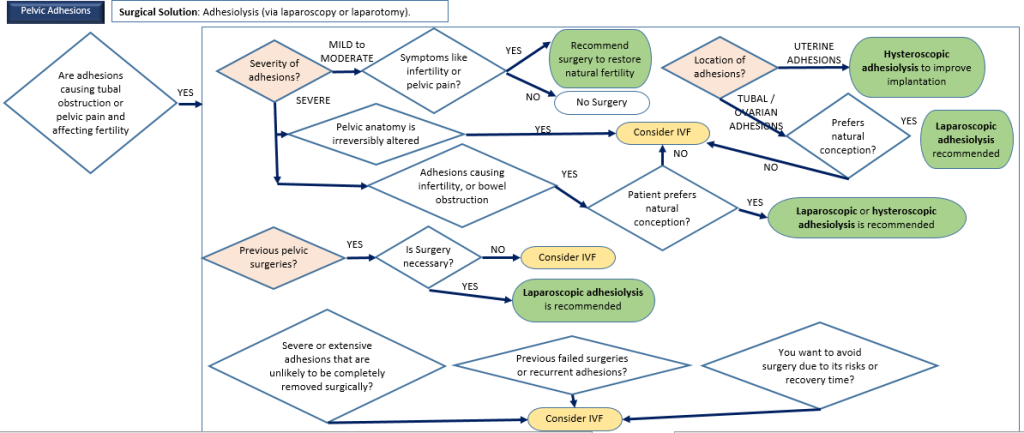
Description: Scar tissue in the pelvic cavity caused by infection, surgery, or endometriosis.
Symptoms: Infertility, chronic pelvic pain, bowel or bladder dysfunction.
Diagnostic Methods: Laparoscopy.
Surgical Options Available: Laparoscopic adhesiolysis.
Alternative Treatments: Pain management, IVF.
Symptoms: Infertility, chronic pelvic pain, bowel or bladder dysfunction.
Diagnostic Methods: Laparoscopy.
Surgical Options Available: Laparoscopic adhesiolysis.
Alternative Treatments: Pain management, IVF.
Potential Adversities of Delaying Surgery
Delaying surgery for pelvic adhesions can lead to:
Progression of adhesions, increasing the severity and complexity of future surgical intervention.
Tubal blockage and infertility, reducing the chances of natural conception.
Chronic pelvic pain, which may become resistant to treatment and reduce quality of life.
Complications like bowel obstruction, which can require emergency surgical intervention.
Recurrent implantation failure or miscarriage if uterine adhesions are involved.
Increased risk of pelvic inflammatory disease (PID) and ectopic pregnancy.
Delaying surgery for pelvic adhesions can lead to:
Progression of adhesions, increasing the severity and complexity of future surgical intervention.
Tubal blockage and infertility, reducing the chances of natural conception.
Chronic pelvic pain, which may become resistant to treatment and reduce quality of life.
Complications like bowel obstruction, which can require emergency surgical intervention.
Recurrent implantation failure or miscarriage if uterine adhesions are involved.
Increased risk of pelvic inflammatory disease (PID) and ectopic pregnancy.
7. Hydrosalpinx 
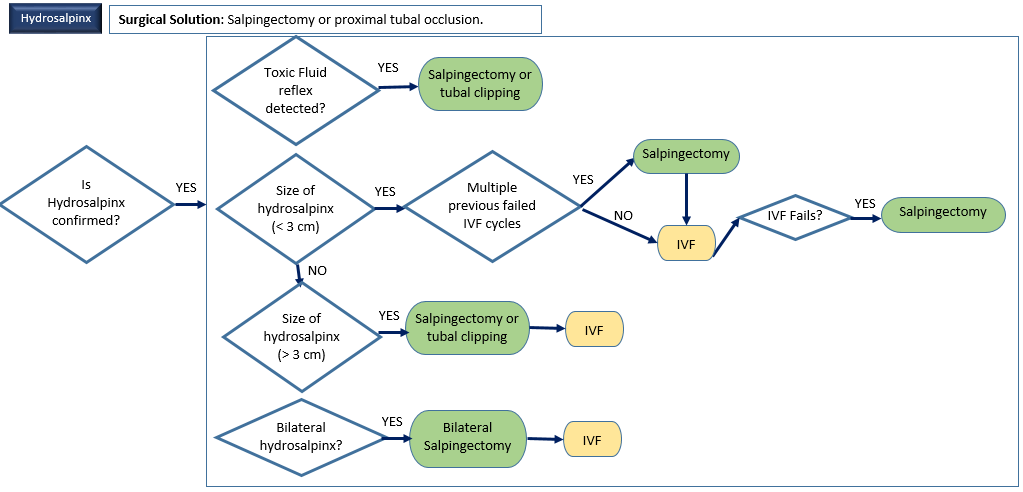
Description: Fluid-filled fallopian tubes caused by infection or inflammation.
Symptoms: Infertility, pelvic pain, abnormal discharge.
Diagnostic Methods: HSG, laparoscopy, ultrasound.
Surgical Options Available: Salpingectomy, proximal tubal occlusion.
Alternative Treatments: IVF post-tubal surgery.
Symptoms: Infertility, pelvic pain, abnormal discharge.
Diagnostic Methods: HSG, laparoscopy, ultrasound.
Surgical Options Available: Salpingectomy, proximal tubal occlusion.
Alternative Treatments: IVF post-tubal surgery.
Potential Adversities of Delaying Surgery
Delaying surgery for hydrosalpinx can lead to:
Repeated IVF failure, as toxic fluid from the hydrosalpinx impairs embryo implantation.
Permanent damage to the endometrium, reducing the success rates of future fertility treatments.
Tubal rupture or pelvic inflammatory disease (PID), which may require emergency surgical intervention.
Chronic pelvic pain and discomfort, lowering quality of life.
Missed opportunities for timely conception, particularly in women with advanced reproductive age or low ovarian reserve.
Delaying surgery for hydrosalpinx can lead to:
Repeated IVF failure, as toxic fluid from the hydrosalpinx impairs embryo implantation.
Permanent damage to the endometrium, reducing the success rates of future fertility treatments.
Tubal rupture or pelvic inflammatory disease (PID), which may require emergency surgical intervention.
Chronic pelvic pain and discomfort, lowering quality of life.
Missed opportunities for timely conception, particularly in women with advanced reproductive age or low ovarian reserve.
8. Congenital Uterine Anomalies 
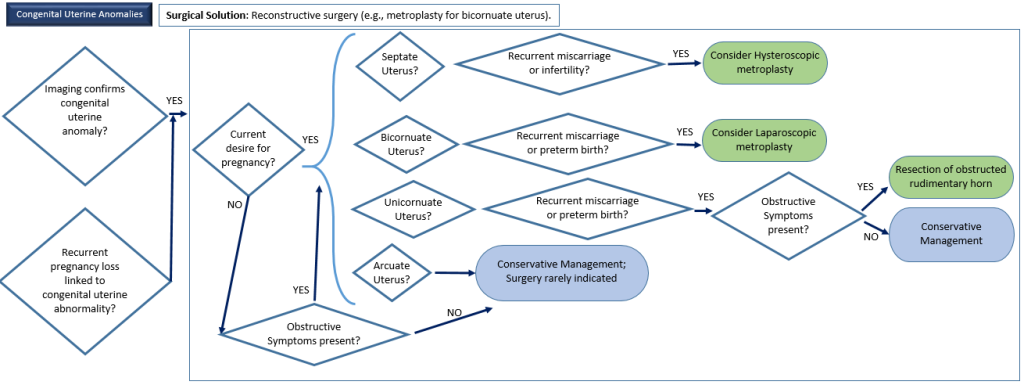
Description: Abnormalities in uterine shape due to incomplete development.
Symptoms: Infertility, recurrent miscarriages, preterm labor.
Diagnostic Methods: 3D ultrasound, MRI, hysteroscopy.
Surgical Options Available: Hysteroscopic or laparoscopic metroplasty.
Alternative Treatments: : IVF for specific anomalies.
Symptoms: Infertility, recurrent miscarriages, preterm labor.
Diagnostic Methods: 3D ultrasound, MRI, hysteroscopy.
Surgical Options Available: Hysteroscopic or laparoscopic metroplasty.
Alternative Treatments: : IVF for specific anomalies.
Potential Adversities of Delaying Surgery
Delaying surgery for congenital uterine anomalies can lead to:
Recurrent miscarriages, preterm birth, and infertility due to structural abnormalities of the uterus.
Chronic pelvic pain and the development of endometriosis in obstructive anomalies.
Increased risk of uterine rupture and severe pregnancy complications if anomalies like a rudimentary horn or bicornuate uterus are left untreated.
Missed opportunities for timely conception, particularly in women with advancing reproductive age.
Emotional and psychological distress due to repeated pregnancy losses and prolonged infertility.
Delaying surgery for congenital uterine anomalies can lead to:
Recurrent miscarriages, preterm birth, and infertility due to structural abnormalities of the uterus.
Chronic pelvic pain and the development of endometriosis in obstructive anomalies.
Increased risk of uterine rupture and severe pregnancy complications if anomalies like a rudimentary horn or bicornuate uterus are left untreated.
Missed opportunities for timely conception, particularly in women with advancing reproductive age.
Emotional and psychological distress due to repeated pregnancy losses and prolonged infertility.
9) Severe Male Factor Infertility 
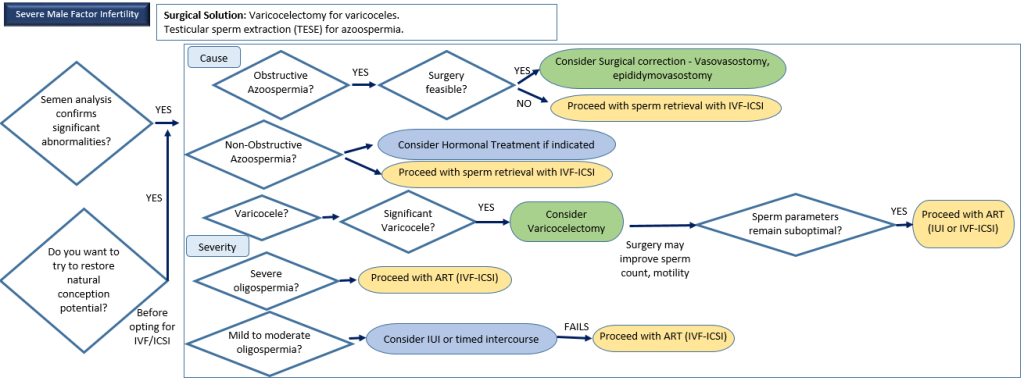
Description: Poor sperm production or quality due to varicocele, azoospermia, or other factors.
Symptoms: Infertility.
Diagnostic Methods: Semen analysis, hormonal tests, scrotal ultrasound.
Surgical Options Available: Varicocelectomy, TESE, vasovasostomy.
Alternative Treatments: IVF-ICSI.
Symptoms: Infertility.
Diagnostic Methods: Semen analysis, hormonal tests, scrotal ultrasound.
Surgical Options Available: Varicocelectomy, TESE, vasovasostomy.
Alternative Treatments: IVF-ICSI.
Potential Adversities of Delaying Surgery
Delaying surgery for severe male factor infertility can lead to:
Irreversible testicular damage, resulting in permanent infertility.
Progressive decline in semen parameters, reducing the chances of natural conception and ART success.
Increased oxidative stress and sperm DNA damage, lowering the likelihood of successful pregnancy even with IVF-ICSI.
Missed opportunities for less invasive treatments, such as IUI or timed intercourse, leading to reliance on more expensive and invasive procedures like IVF-ICSI.
Emotional and psychological distress, as prolonged infertility can cause significant strain on relationships and mental health.
Delaying surgery for severe male factor infertility can lead to:
Irreversible testicular damage, resulting in permanent infertility.
Progressive decline in semen parameters, reducing the chances of natural conception and ART success.
Increased oxidative stress and sperm DNA damage, lowering the likelihood of successful pregnancy even with IVF-ICSI.
Missed opportunities for less invasive treatments, such as IUI or timed intercourse, leading to reliance on more expensive and invasive procedures like IVF-ICSI.
Emotional and psychological distress, as prolonged infertility can cause significant strain on relationships and mental health.
10. Intrauterine Adhesions (Asherman’s Syndrome)

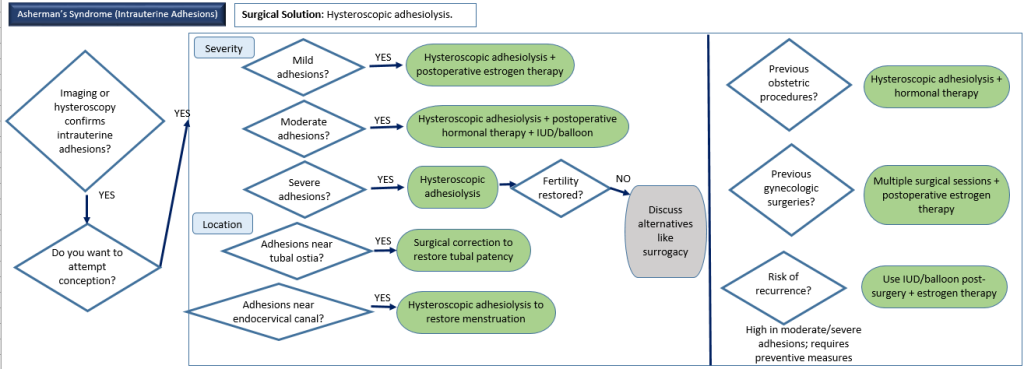
Description: Scar tissue in the uterine cavity caused by trauma or infection.
Symptoms: Infertility, irregular periods, recurrent miscarriages.
Diagnostic Methods: Hysteroscopy, ultrasound.
Surgical Options Available: Hysteroscopic adhesiolysis.
Alternative Treatments: IVF (if severe scarring persists).
Symptoms: Infertility, irregular periods, recurrent miscarriages.
Diagnostic Methods: Hysteroscopy, ultrasound.
Surgical Options Available: Hysteroscopic adhesiolysis.
Alternative Treatments: IVF (if severe scarring persists).
Potential Adversities of Delaying Surgery
Delaying surgery for intrauterine adhesions can lead to:
1) Progression of adhesions, increasing the severity and complexity of future surgical interventions.
2) Chronic infertility and recurrent miscarriages due to impaired implantation and reduced uterine cavity size.
3) Permanent damage to the endometrial lining, reducing the chances of future pregnancies even with assisted reproductive technologies.
4) Tubal blockage and cervical stenosis, causing additional complications such as hydrosalpinx, dysmenorrhea, and hematometra.
5) Increased surgical risks and need for multiple surgeries if adhesions are allowed to reform or worsen.
6) Missed opportunities for simpler corrective procedures, potentially requiring more invasive options like surrogacy if fertility cannot be restored.
Delaying surgery for intrauterine adhesions can lead to:
1) Progression of adhesions, increasing the severity and complexity of future surgical interventions.
2) Chronic infertility and recurrent miscarriages due to impaired implantation and reduced uterine cavity size.
3) Permanent damage to the endometrial lining, reducing the chances of future pregnancies even with assisted reproductive technologies.
4) Tubal blockage and cervical stenosis, causing additional complications such as hydrosalpinx, dysmenorrhea, and hematometra.
5) Increased surgical risks and need for multiple surgeries if adhesions are allowed to reform or worsen.
6) Missed opportunities for simpler corrective procedures, potentially requiring more invasive options like surrogacy if fertility cannot be restored.